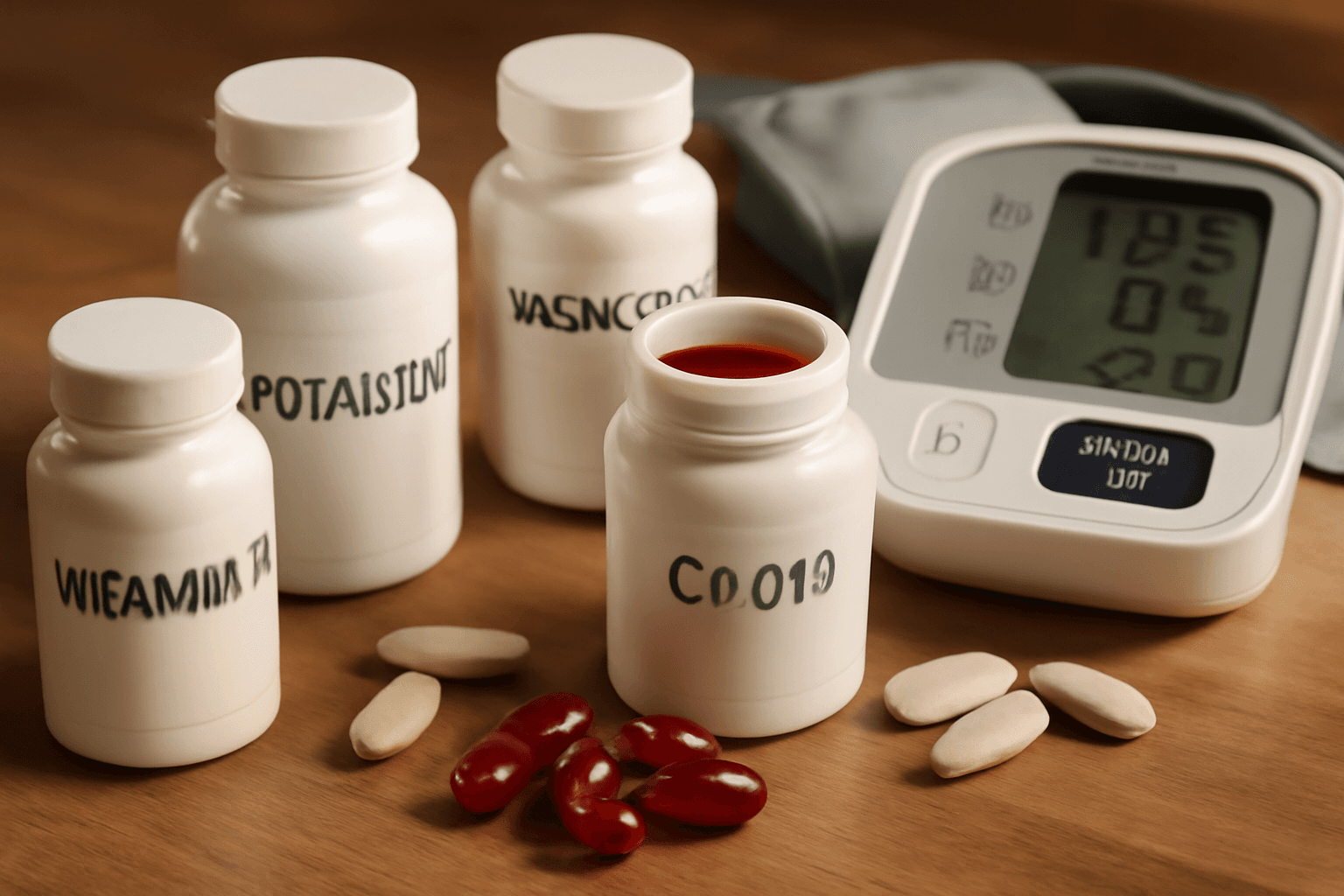
Cardiovascular disease is one of the leading causes of death worldwide. In South Korea's mortality statistics, heart disease ranks among the top causes of death, and the most effective way to prevent it is through dietary improvements. By consuming the right nutrients and improving lifestyle habits, you can significantly enhance cardiovascular health. This article will provide detailed information about specific food choices, lifestyle habits, and necessary supplements for heart health.
Foods That Are Good for Your Heart
The key to a heart-healthy diet is choosing foods that reduce inflammatory responses and maintain vascular health. Research shows that the Mediterranean diet reduces the risk of heart disease by 30%, demonstrating how important the selection of specific food groups is.
Foods Rich in Omega-3 Fatty Acids
Omega-3 fatty acids (EPA and DHA) found in oily fish reduce blood triglycerides by 20-30% and improve endothelial function in blood vessels. Salmon, mackerel, sardines, and anchovies are recommended 2-3 times per week. Consuming about 100g of fish per serving provides sufficient omega-3. If fish is not consumed, flaxseeds, nuts (especially walnuts), and chia seeds can serve as alternatives, though plant-based omega-3 has lower bioavailability than animal-based sources, requiring larger quantities.
Correct Choices of High-Protein Foods
Protein is essential for maintaining muscle and vascular elasticity. However, red meat high in saturated fat increases the risk of heart disease, so poultry (chicken breast, turkey) and legumes (black beans, lentils, chickpeas) should be prioritized. Every 100g of beans provides about 15g of protein along with 7g of dietary fiber, effectively lowering cholesterol. Eggs are also a good choice, particularly lutein in egg yolks, which supports vascular health.
Vegetables and Fruits Rich in Potassium
Potassium plays a key role in lowering blood pressure by promoting sodium excretion. Bananas contain 358mg of potassium per 100g, while spinach (558mg), sweet potatoes (460mg), and avocados (485mg) are also excellent sources of potassium. The daily recommended potassium intake for adults is 3,500-4,700mg, which can be met through a variety of vegetables and fruits. Those with kidney disease should consult with healthcare providers to adjust potassium intake.
Foods Rich in Antioxidants
Berries (blueberries, strawberries, black grapes) contain anthocyanins and polyphenols that reduce vascular inflammation. Research shows that consuming one cup (about 150g) three to four times a week reduces cardiovascular disease risk by 15%. Flavonoids in dark chocolate (70% cacao or higher) promote vascular dilation, with a daily intake of 20-30g being appropriate. Lycopene in tomatoes and beta-carotene in carrots also support vascular health through antioxidant functions.
Whole Grains and Dietary Fiber
Refined carbohydrates should be replaced with whole grains like brown rice, oats, and barley, as they cause blood vessel damage through blood sugar spikes. One cup of oats (about 40g) provides 10g of dietary fiber, reducing LDL cholesterol by 5-10%. Simply starting each morning with oatmeal can have long-term positive effects on cardiovascular health.
Lifestyle Habits Good for Heart Health
Lifestyle habits are just as important as diet. Physical activity, stress management, and sleep are key factors that determine cardiovascular health. These work through various mechanisms including improving endothelial function, regulating blood pressure, and reducing inflammation.
Regular Aerobic Exercise
Thirty minutes of moderate-intensity aerobic exercise (brisk walking, jogging, swimming) five or more days a week reduces cardiovascular disease risk by 35%. During exercise, heart rate should be maintained at 50-70% of maximum heart rate, with intensity gradually increased according to individual fitness levels. Incorporating resistance training two to three days a week also improves metabolic health and enhances vascular function.
Stress Management's Impact on Cardiovascular Health
Chronic stress triggers increased cortisol hormone levels, causing vascular constriction and inflammation. This raises blood pressure and increases the risk of blood clot formation. Meditation, yoga, and deep breathing exercises activate the parasympathetic nervous system, lowering heart rate and relaxing blood vessels. Just 10-20 minutes of daily mindfulness meditation can reduce blood pressure by about 5mmHg, equivalent to medication therapy. Listening to music, forest therapy, and social activities with friends are also effective for stress reduction.
The Importance of Adequate Sleep
Sleep deprivation (six hours or less per day) raises blood pressure and increases inflammatory markers. Seven to nine hours of quality sleep normalizes the autonomic nervous system and restores endothelial function. If sleep apnea is present, blood pressure rises further, requiring medical diagnosis and treatment. Going to bed and waking at consistent times and reducing screen exposure one hour before bed improve sleep quality.
Smoking Cessation and Alcohol Moderation
Smoking damages the vascular endothelium and increases platelet aggregation, raising blood clot formation risk four-fold. One year after quitting smoking, cardiovascular disease risk decreases by 50%, and after 15 years, it returns to the level of non-smokers. Alcohol consumption should be limited to no more than two drinks per day for men and one drink per day for women. Excessive drinking causes cardiac arrhythmias, high blood pressure, and increased triglycerides.
4 Supplements That Support Heart Health
When it's difficult to obtain all necessary nutrients from diet alone, scientifically-supported supplements can be considered. However, supplements are not medications, and consultation with healthcare providers is essential to check for interactions with existing medications.
Magnesium: Vascular Relaxation and Blood Pressure Regulation
Magnesium acts as a calcium antagonist, relaxing vascular smooth muscle and lowering blood pressure. According to meta-analyses, daily magnesium supplementation of 200-400mg reduces systolic blood pressure by 3-4mmHg. The effect is more pronounced in cases of magnesium deficiency. While magnesium can be obtained from foods like spinach, pumpkin seeds, and almonds, glycinate or taurate forms of supplements have better absorption when intake is insufficient. Excess intake may cause diarrhea, so daily intake should not exceed 350mg for adults.
Vitamin D: Reducing Vascular Inflammation and Immune Regulation
Vitamin D deficiency is associated with vascular stiffness and increased inflammation. When blood vitamin D levels fall below 30ng/mL, cardiovascular disease risk significantly increases. Daily vitamin D supplementation of 1,000-2,000IU improves endothelial function and lowers blood pressure. Supplementation is especially recommended during winter or for those with limited outdoor activity. Determining dosage based on individual deficiency levels measured through blood tests (25-OH vitamin D) is most effective.
Vitamin K: Preventing Vascular Calcification
Vitamin K2 prevents calcium deposition in arterial walls, delaying atherosclerosis. Daily vitamin K intake (K1 and K2 combined) of 45-90mcg reduces vascular stiffness. Leafy green vegetables (kale, broccoli) contain primarily vitamin K1, while vitamin K2 is found in fermented foods (natto, kimchi) and some cheeses. For those taking anticoagulants like warfarin, vitamin K intake should be kept consistent to maintain stable medication effects.
Coenzyme Q10 (CoQ10): Cellular Energy and Antioxidant Protection
CoQ10 promotes ATP production within mitochondria, enhancing myocardial contractility. It also serves as a potent antioxidant, preventing LDL oxidation. For those with high blood pressure or taking statin medications, daily CoQ10 supplementation of 100-200mg lowers blood pressure by about 10mmHg and improves cardiac function. Since statin drugs suppress CoQ10 production, supplementation is especially recommended for patients on long-term therapy. Being fat-soluble, absorption improves when taken with dietary fat.
The Impact of Heart Health on Overall Health
Cardiovascular health extends far beyond preventing heart disease, having broad implications for overall bodily health and lifespan. A healthy cardiovascular system delivers adequate oxygen and nutrients to all organs including the brain, kidneys, and muscles, which is essential for cognitive function, kidney function, and maintaining body composition.
Cognitive Function and Brain Health
Cardiovascular health and brain health are closely connected. Vascular cognitive decline results from neurological damage caused by reduced blood flow to the brain. High blood pressure, blood sugar, and cholesterol accelerate damage to brain microvasculature, increasing Alzheimer's disease risk. Simply maintaining heart health can reduce the risk of cognitive decline after age 65 by 30%. Omega-3 and magnesium also provide neuroprotective effects, so a heart-healthy diet simultaneously supports brain health.
Preserving Kidney Function
High blood pressure is a major cause of damage to the glomeruli's microvasculature in the kidneys. When diabetes and high blood pressure coexist, kidney damage risk significantly increases. Controlling blood pressure to 120/80mmHg or below can slow the progression of kidney disease by 50%. Managing blood pressure through potassium intake, reducing salt consumption, and regular exercise both preserve kidney health and improve heart health. As kidney disease progresses, cardiovascular disease risk increases dramatically, making early prevention particularly important.
Body Composition and Metabolic Health
A heart-healthy diet (high protein, low salt, abundant dietary fiber) naturally promotes weight loss and muscle maintenance. A weight loss of just 5-10% reduces blood pressure by 5-20mmHg, improves blood sugar control, and decreases inflammatory markers. Regular exercise is particularly effective at reducing visceral fat, which directly decreases vascular inflammation. When metabolic health improves, the risk of not only cardiovascular disease but also type 2 diabetes, fatty liver disease, and cancer simultaneously decreases.
Lifespan and Quality of Life
According to the Framingham Heart Study, managing cardiovascular risk factors (blood pressure, cholesterol, smoking) is the most effective method of extending lifespan. People with excellent cardiovascular health live an average of 10 years longer, with particularly high quality of life in their senior years. Independent living, maintaining cognitive function, and preserving physical activity capacity are all linked to cardiovascular health. Therefore, managing heart health is far more than disease prevention—it is a fundamental investment in a fulfilling life.
Summary
Key foods for cardiovascular health: Prioritize oily fish (2-3 times per week), legumes, whole grains, berries, nuts, and potassium-rich vegetables. Limit saturated fats, processed foods, and high-salt foods.
The importance of lifestyle habits: Thirty minutes of moderate-intensity aerobic exercise five days per week, seven to nine hours of daily sleep, and stress management (meditation, yoga) provide medication-level effects. Smoking cessation and alcohol moderation are essential.
Supplement use: Magnesium (blood pressure regulation), vitamin D (inflammation reduction), vitamin K (preventing vascular calcification), and CoQ10 (cardiac function) can be considered when inadequate from diet alone, but decisions should be made in consultation with healthcare providers considering individual health status and current medications.
Broad health benefits: Improved cardiovascular health leads to better brain health, kidney function, metabolic health, and extended lifespan. Preventive management is far more effective and economical than disease treatment.
Medical disclaimer: The information in this article is for general educational purposes and may apply differently depending on individual health conditions. Particularly for those with existing cardiovascular disease, blood sugar regulation disorders, kidney disease, or those taking medications, consultation with healthcare professionals (physicians or nutritionists) is essential to establish personalized diet and exercise plans. Supplements are not medications and may interact with existing drugs, making professional approval essential.